Diabetes Beta Cell - Insulin (β cells)
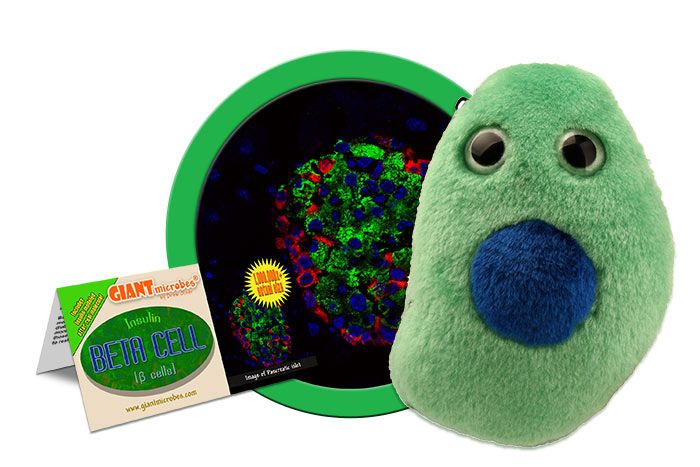
Pancreatic beta cells produce insulin which regulate sugar levels in the body. Learn how they work and what happens when they don't with this adorable plush.
GIANTmicrobes Diabetes plush is cuddly and includes an insulin piece. Memorable gift for diabetics, friends, family, healthcare and anyone with a healthy sense of humor. Fun hands-on-way to learn about Diabetes, the Pancreas and human biology.
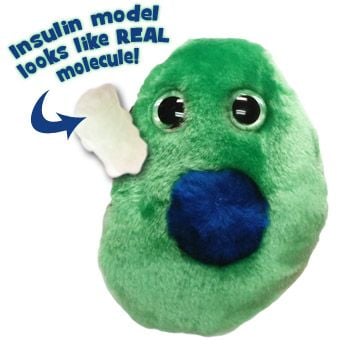
Each plush cell contains a 3” zippered pouch. Inside you’ll find an Insulin plush piece modeled from the actual insulin molecule. Also includes an educational card with fascinating facts! Pairs well with our Pancreas plush.
Size: 6 x 4 x 2”
Product Details
Additional Information
| Sizes | Giantmicrobes are based on actual microbes, cells, organisms and other critters, only 1,000,000 times actual size! Gigantic (GG) 16-24" XL (XL) 10-15" Original (PD) 5-8" Keychain (KC) 2-4" with clip |
|---|---|
| Materials | Plush from all new materials. Stuffed with polyester fiber fill. Surface washable: sponge with water & soap, air dry. |
| Packaging | Each plush microbe includes a printed card with fun, educational and fascinating facts about the actual microbe or cell. |
| Safety | Every product meets or exceeds U.S. and European standards for safety. For ages 3 and up. |
All about Diabetes Beta Cell - Insulin (β cells)
Pancreatic beta cells produce the insulin that helps regulate the level of glucose sugar in the body. When blood sugar levels rise, beta cells release insulin which causes fat and muscle cells to begin absorbing the excess sugar. As a result, glucose levels return to healthy levels – and the sugar is stored for later use as a cellular energy source.
However, if the beta cells are damaged, insulin production can become impaired. Type 1 diabetes is believed to be the result of an autoimmune response where the body’s own immune system attacks the cells and destroys them. Because the body is no longer able to produce insulin and reduce its sugar levels effectively, glucose levels rise. Increased fluid ingestion typically results, as well as frequent urination as the body struggles to reduce sugar levels. (The excess glucose also imparts a sweet taste to the body’s aqueous excretions, which is how diabetes was historically diagnosed...)
Even if the beta cells are still functioning, diabetes can still occur if the body’s fat and muscle cells become insufficiently responsive to insulin – or if insufficient quantities are produced. This Type II diabetes is far more common, and typically occurs in adults.
But fortunately, Type II diabetes can typically be managed with dietary modifications, exercise, and sometimes medication. And while Type I diabetes requires the regular injection of insulin, rapid developments in monitoring and delivery mechanisms have greatly improved the lives of those living with diabetes – and biological research is honing in on ways to restore damaged beta cells and cure diabetes for good.
| Description | Beta Cells are found in islets of Langerhans, which are patches of endocrine tissue in the pancreas. They make up 65-80% of the cells in those islets. Their main function is to produce insulin, a hormone that tells your body cells to absorb glucose so that it does not remain in the blood. This regulates blood glucose levels. |
|---|
| Name | Scientists discovered an extract that had antidiabetic properties, and they hypothesized that the antidiabetic hormone in its pure form came from the insular tissues of the pancreas, which would later be recognized as the islets of Langerhans. This insular derivation caused the scientists to name the substance, that had yet to be isolated, insulin. |
|---|
| Actual Size | 10 microns, 1/10 the thickness of a piece of paper. |
|---|
| System | Endocrine System |
|---|
| Quantity | For a rough estimation, say 75% of cells in islets are beta cells. 1 million islets x 1000 average cells in an islet x 0.75 = 750 million beta cells. |
|---|
| History |
1869: Paul Langerhans was the first to describe the islets of Langerhans, which bear his name. 1921: Frederick Grant Banting and Charles Herbert Best discovered insulin. |
|---|
| Fascinating Facts |
Islets: A healthy, adult pancreas has about 1 million islets. Each islet contains on average 1000 cells. Celebrities with Diabetes: Tom Hanks, Paula Deen, and Halle Berry all have Type 2 Diabetes. |
|---|