ADHD
GIANTmicrobes ADHD is a plush representation of Attention Deficit Hyperactivity Disorder. This product helps educate, spread awareness, and encourage discussions about vitally important topics in mental health.
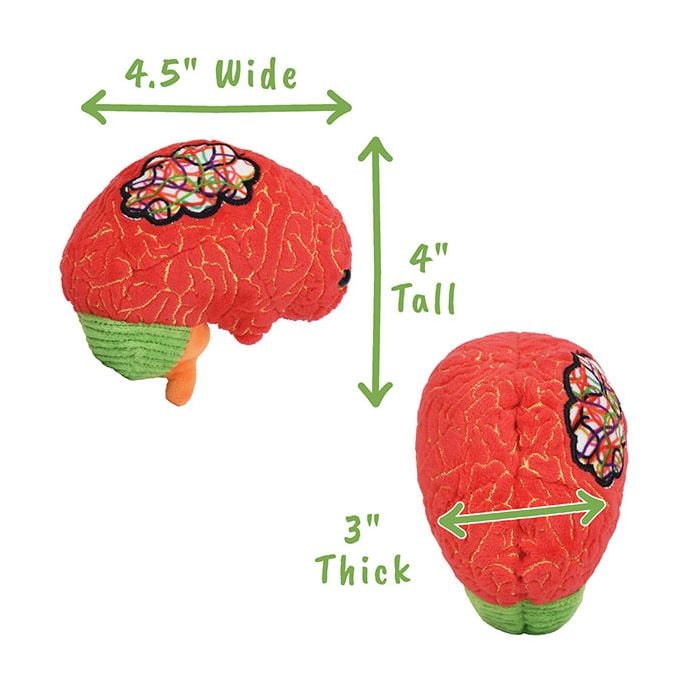
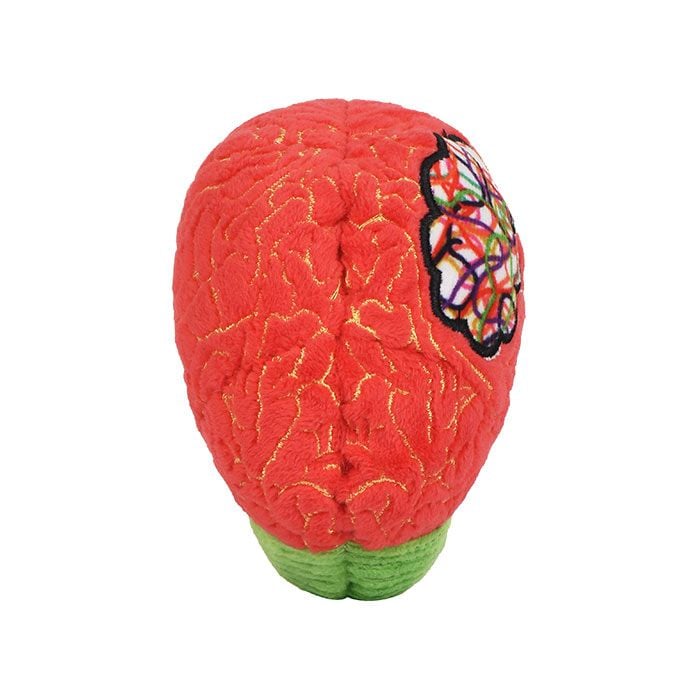
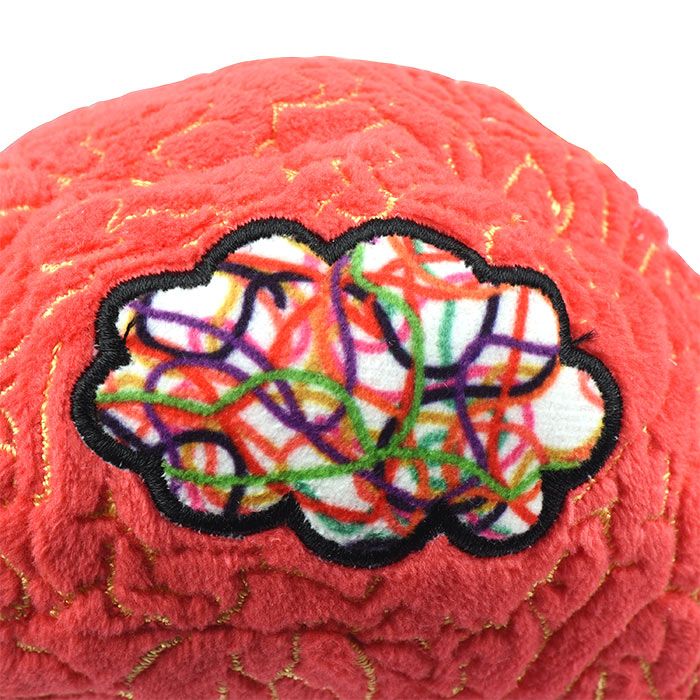
This soft, cuddly representation makes a memorable emotional support and educational gift for loved ones dealing with ADHD. Features a brain with a thought cloud, embroidered details of the cerebrum and cerebellum and includes a printed card with educational facts to help spark discussions.
For families, students, therapists, social workers, healthcare workers and psychologists - this is a unique, memorable and useful tool to help educate, spread awareness, and get more people talking about mental health.
Size: 4.5 x 4 x 3"
Product Details
Additional Information
| Sizes | Giantmicrobes are based on actual microbes, cells, organisms and other critters, only 1,000,000 times actual size! Gigantic (GG) 16-24" XL (XL) 10-15" Original (PD) 5-8" Keychain (KC) 2-4" with clip |
|---|---|
| Materials | Plush from all new materials. Stuffed with polyester fiber fill. Surface washable: sponge with water & soap, air dry. |
| Packaging | Each plush microbe includes a printed card with fun, educational and fascinating facts about the actual microbe or cell. |
| Safety | Every product meets or exceeds U.S. and European standards for safety. For ages 3 and up. |
All about ADHD
FACTS: Attention deficit hyperactivity disorder, or ADHD, is a common mental health issue. Symptoms include inattention, hyperactivity and impulsivity. Parents may notice these symptoms in toddlers, but ADHD cannot be properly identified until age four. The disorder is often diagnosed during elementary school when it becomes more apparent that a child does not pay attention or moves excessively. For teens and adults, symptoms of hyperactivity such as fidgeting, restlessness, impulsivity and impatience may be more pronounced.
ADHD is also considered a form of neurodivergence, the concept that there are a variety of ways that people's brains process information, function, and present behaviorally. Neurodiversity recognizes that both brain function and behavioral traits are simply indicators of how diverse the human population is. Thanks to their creative thinking, people with ADHD are often good problem solvers, energetic, and sensitive to others. Correct diagnosis of ADHD can be perplexing since many of the core symptoms are similar to everyday childhood behaviors. It may be difficult to distinguish between normal age-appropriate emotional growth and evidence of ADHD. As with many mental health conditions, there is no definitive way to diagnose ADHD.
Some professionals believe that ADHD has been overdiagnosed. The rising number of ADHD cases in recent decades is staggering. In the 1970s about 1% of kids were considered to have ADHD. By the 1990s the rate was over 3%. Today ADHD is thought to impact 5% of children and 2% of adults. It is about twice as prevalent in boys than girls. Even though some people are misdiagnosed, there is no doubt that ADHD is real.
Treatment is key to minimize the risk for social and learning problems. It is best not to seek simple explanations and proposed medical remedies that promise fast results. Most important is to learn about ADHD, consult with professionals and evaluate the options. Behavior therapy focuses on helping people learn how to control their behavior. Medication can also improve the symptoms, especially when combined with therapy. Along with treatment, ways to cope include keeping routines, avoiding distractions, and finding support with community groups and healthcare professionals.